Your comfort and dignity are important to us.
We are committed to putting patients at ease and if you wish a chaperone to be present during your examination, please do not hesitate to ask a member of our reception team or a clinician. A chaperone is available for any consultation, examination, or procedure if you would like one.
✔You can request a chaperone at any time
✔They are here to support you and ensure your comfort
✔Please let the clinician or receptionist know
We respect that patients may have cultural, religious or gender preferences for their chaperone. Please let us know your preference and we will do our best to accommodate this.
Just ask – we are happy to help.
The Grove Medical Group is committed to providing a safe and comfortable environment in which both patients and staff can feel confident that best practice is consistently upheld. The safety and wellbeing of everyone involved is of paramount importance. A chaperone is present to support and safeguard both the patient and the clinician, and to act as an impartial observer, ensuring that ongoing consent is maintained throughout the procedure.
Patients are entitled to request a chaperone at any time. Information about the availability of chaperones is provided on our website, within the patient waiting area, and in all clinical consultation rooms. We recognise that patients may have cultural, religious, or gender preferences regarding who acts as their chaperone. We encourage patients to let us know their preference, and we will try our best to accommodate them.
The Grove Medical Group Chaperone Policy – updated April 2026
Who can act as a chaperone
At The Grove Medical Group, it is policy that any member of the team can act as a chaperone.
However, they must have undertaken chaperone training and have undergone a DBS check.
Chaperone training which should include:
- what is meant by the term chaperone
- what is an ‘intimate examination’
- why chaperones need to be present
- the rights of the patient
- their role and responsibilities. It is important chaperones should place themselves inside the screened-off area rather than outside of the curtains/screen
- policy and mechanism for raising concerns.
As per the GMC guidance, relatives or friends of the patient are not considered to be an impartial observer so would not usually be a suitable chaperone but staff at this practice should comply with a reasonable request to have such a person present in addition to the chaperone.
Role and expectations of a chaperone
Staff acting as a chaperone should be present throughout the entire examination. They should understand the nature of the examination and respect the patients dignity and confidentiality. Chaperones must be prepared to raise concerns if needed. Concerns can be raised with the clinician, a Senior Partner or the Practice Manager.
When a chaperone is unavailable
If either the clinician or the patient does not want the examination to go ahead without a chaperone present, or if either is uncomfortable with the choice of chaperone, the clinician may offer to delay the examination until a later date when a suitable chaperone will be available providing the delay would not adversely affect the patient’s health.
When a patient refuses a chaperone
If the clinician does not want to proceed with the examination without a chaperone but the patient has refused a chaperone, the clinician must clearly explain why they want a chaperone to be present. The GMC states that ultimately the patient’s clinical needs must take precedence. The clinician may wish to consider referring the patient to a colleague who would be willing to examine them without a chaperone providing a delay would not adversely affect the patient’s health.
Home visits and chaperones
Healthcare professionals working alone, especially during intimate examinations or in isolated settings like a patient’s home, face increased risk of their actions being misinterpreted. To mitigate this, they should offer a chaperone in advance of the appointment where possible. Where this is not possible, they should ensure clear communication and thorough documentation explaining why the examination proceeded without a chaperone present and that this was agreed with the patient.
Vulnerable patients
If the patient cannot make an informed decision, the healthcare professional must use their clinical judgement and be able to justify their course of action. The practice will ensure that reasonable adjustments are made for vulnerable patients.
Children and young people under 18 years
Intimate examination on children and young people under 18 years should be carried out in the presence of a formal chaperone, this protects both patient safety and professional standards. This applies even when a parent or guardian is present. Parents or guardians must receive an appropriate explanation of the procedure to provide informed consent when the young person is unable to do so themselves.
Chaperone Quick Guide
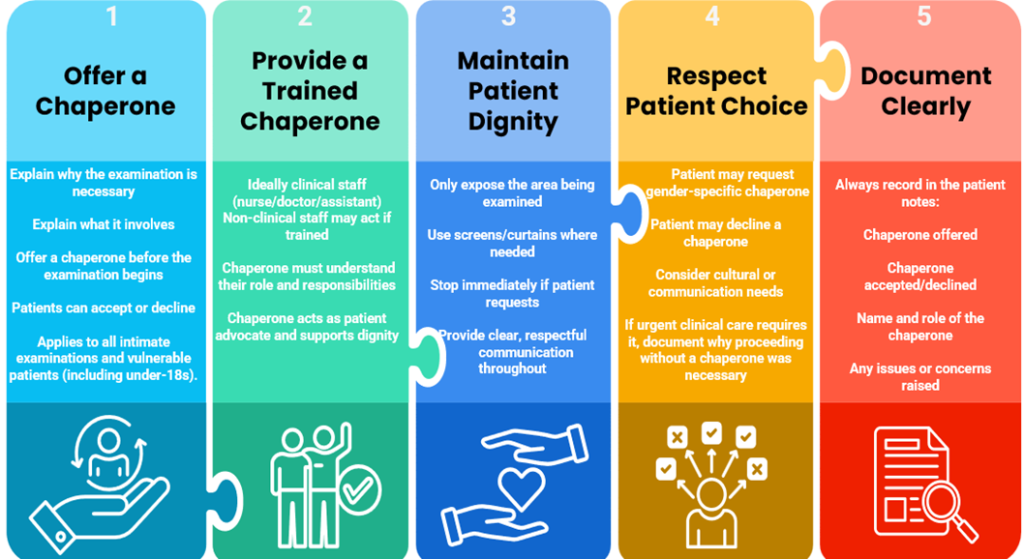
Further guidance in relation to chaperoning can be found below
NHS England » Improving chaperoning practice in the NHS: key principles and guidance
